
For World COPD Day 2018 and the publication of Life of Breath’s new Policy Report, consultant respiratory physician and honorary senior lecturer at the Academic Respiratory Unit (University of Bristol) Dr James Dodd writes…
What is COPD?
Chronic Obstructive Pulmonary Disease (COPD) is an umbrella term which includes ‘chronic bronchitis’ and ‘emphysema’, it causes a progressive decline in lung function and health. It is common, effecting 2% of the adult population and is projected to become the 3th leading cause of death in the UK. People with COPD experience breathlessness, cough and wheeze and often suffer with repeated chest infections, these ‘exacerbations’ are the 2nd most common reason for emergency admissions to hospital.
Sadly, around 2 of the 3 million people with COPD in the UK remain undiagnosed, meaning that they live with debilitating symptoms for many years before receiving the support and advice they need. These ‘missing millions’ are the driving force behind COPD awareness month and World COPD Day.
It is not known for sure why just 1 out of 3 people with COPD have been formally diagnosed, but is likely to be a combination insufficient training and resources to ensure healthcare professionals diagnose COPD early and under reporting by patients. As a COPD doctor I appreciate how the stigma of smoking and sense of guilt reported by people play an important role in delayed presentation to healthcare professionals. So my message is if you are breathless please pop in to your GP for a chat or take the British Lung Foundation ‘Breath Test’. You will not be judged and there is lots we can do to help.
How do I get COPD?
It is also important to recognise that COPD is a disease of health inequality, disproportionately affecting those in society most economically and socially disadvantaged, compounding the difficulties they face in accessing the support they need. Smoking, outdoor air pollution and housing are all thought to be factors driving these inequalities.
In the UK the majority of people develop COPD from cigarette smoking, but recent studies suggest that other factors such as air pollution also have a significant and increasing role to play. Early life exposure to smoking and pollution are thought to increase the risk of COPD by stunting lung development during childhood. Building on this research, we hope to work with population scientists and clinicians in Bristol and Leicester to test new ways of detecting COPD early.
 Air pollution in London
Air pollution in London
As well as contributing to developing COPD, air pollution is also important for people living with COPD now. Invisible levels of pollution breach safe limits in most UK major cities and are estimated to result in 40,000 avoidable deaths a year (300 a year in Bristol alone). People with lung diseases such as COPD are particularly vulnerable, the main sources of pollution appears to be from traffic, especially diesel engines.
Domestic sources of air pollution are also important and I was shocked to learn that even new ‘eco’ Woodburners are equivalent to 6 diesel trucks or 18 modern diesel cars outside your home! Here at Southmead Hospital in Bristol, we would like to lead by example and our fantastic sustainable healthcare team have been working with us to look at ways we can be less polluting and more healthy. A number of initiatives from electric bikes and hybrid cars for staff travel to looking at new sustainable respiratory pathways of care are designed to make a difference to our environment for our staff and patients.
How do you treat COPD?
For many years following the early descriptions of COPD there was a sense of nihilism, with medical professionals often frustrated by the seemingly limited treatment options. There is reason to be hopeful, however, as we recognise the value of making sure we provide evidence-based ‘bundles’ of care not just restricted to inhalers, but ensure we deliver smoking cessation, flu vaccination and pulmonary rehabilitation.
Pulmonary rehabilitation in particular deserves special mention. This personalised education and exercise programme is delivered in groups over a 6 week period and has wonderfully robust evidence of effects across the board in COPD – helping people manage breathlessness, increase exercise capacity and tackle anxiety and depression, both of which are so common in COPD.
You can learn more about our pulmonary rehabilitation service ‘LEEP’ Lung Exercise and Education Programme here . I am particularly pleased that our team at Southmead Hospital are now able to provide another new treatment for our patients with severe emphysema, known as bronchoscopic lung volume reduction. This NICE approved treatment is delivered through an endoscope to reduce the volume of damaged and overinflated lung by placing one way valves in the airways. These endobronchial valves offer new hope to patients with otherwise limited treatment options and who remain severely disabled by breathlessness and limited exercise capacity.
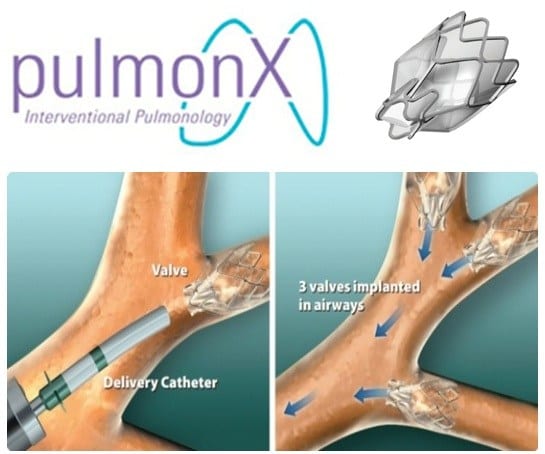
Endobronchial one-way valves are about the size of a pencil head and inserted into the airways of the damaged lung (Image: pulmonX Zephyr EBV)
Breathlessness Research
Breathlessness is a universal experience of patients living with COPD. It is also a very personal experience. Some people deal with breathlessness better than others. As a result, doctors find it hard to measure and difficult to treat. Those living with breathlessness are often forgotten. We want to help people live well with breathlessness. That is why I have been so pleased to be part of the unique Life of Breath research project.
This group, led by Prof Havi Carel and Prof Jane Macnaughton brings together philosophers, anthropologist, history and literature scholars and more. The project recognises that breathing isn’t just a bodily function. It allows us to speak, laugh and sing. It connects us to the outside world. It reflects our state of mind and can be consciously controlled. Breath has inspired art and literature. For many it has spiritual significance. The personal and cultural meaning of breathing goes beyond the simple act of keeping us alive.
Today we are pleased to release some of our findings and policy recommendations in a new PolicyBristol report: “More than a medical symptom: the need for holistic care of breathlessness”
Life of Breath policy report
http://www.bristol.ac.uk/policybristol/policy-briefings/life-of-breath/
(Blog header image by Jordan Collver. Breathlessness is a complex and subjective experience).
James Dodd
James is a Consultant Senior Lecturer in Respiratory Medicine at the Academic Respiratory Unit, University of Bristol. His research focuses on the multi-system impact of lung disease and his clinical work is at Southmead Hospital, Bristol, where he has responsibility for the care of patients with complex COPD and asthma.
http://www.bristol.ac.uk/clinical-sciences/people/james-w-dodd/index.html
Republished by kind permission of the author. View the original article
